Vascular Conditions We Treat in Fayetteville, NC
Dr. Leke and his team provide expert care for varicose veins, spider veins, leg pain, leg swelling, venous ulcers, and deep vein thrombosis (DVT). Using advanced imaging and minimally invasive techniques, we help patients find long-term relief from painful and unsightly vein disorders.
Varicose Veins, Spider Veins & Venous Insufficiency Treatments
Our specialists focus on improving both the function and appearance of your legs through personalized vein treatments. We use noninvasive diagnostic tools and endovascular procedures to effectively manage venous insufficiency and restore proper blood flow.
Dr. Leke’s approach minimizes downtime and maximizes results, helping patients experience lasting comfort and confidence.
Common Causes of Vein Disease and Venous Disorders
The most common contributors to varicose and spider vein formation include a sedentary lifestyle, obesity, pregnancy, and occupations requiring prolonged standing or sitting. Genetics can also play a major role—many people develop vein disease even without these risk factors.
Venous insufficiency and varicose veins are most often seen between ages 30 and 70, though they can occur at any age. Pregnancy frequently contributes to these issues due to increased venous pressure and hormonal changes that prepare the body for childbirth.
Signs and Symptoms of Varicose Veins
Varicose veins often appear as twisted, bluish veins beneath the skin. Common symptoms include leg cramps, burning or itching sensations, heaviness, and restlessness in the legs. In more advanced stages, skin discoloration may occur due to inflammation or scratching.
If you recognize these signs, schedule a vein evaluation with Dr. Leke to receive a personalized treatment plan for your condition.
Carotid Artery Disease & Stroke Prevention
The carotid arteries carry blood to the brain and face. When plaque builds up and narrows these arteries—a condition known as carotid artery disease—the risk of stroke increases significantly.
Our clinic offers ultrasound screenings to detect carotid disease early, allowing for timely intervention and proactive stroke prevention.
Dialysis Access Creation & Vascular Access Management
We specialize in dialysis access placement and ongoing care, including AV grafts and AV fistulas. Regular evaluations ensure proper blood flow and prevent complications, maintaining reliable access for effective dialysis.
Our vascular team prioritizes precision, patient comfort, and long-term access success.
Lymphedema Diagnosis & Treatment
Lymphedema develops when lymphatic fluid builds up in the body’s soft tissues—often in an arm or leg—causing swelling, tightness, and heaviness. Symptoms may take years to appear after lymphatic injury but can progress without proper management.
Common warning signs include reduced flexibility, skin redness, or difficulty wearing rings or shoes. We provide comprehensive lymphedema care to improve circulation, reduce swelling, and restore mobility.
Frequently Asked Questions
What are varicose veins and venous disease?
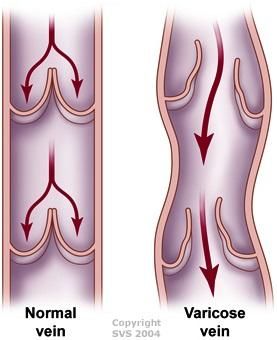
Circulation in the human body occurs in a loop with blood carried from the left ventricle of the heart to your tissues through arteries and then returned to the heart through veins. The arteries benefit from the pumping action of your heart but not so for the veins. As a result of the lack of that propulsive force in veins blood flow within veins is quite sluggish when compared to arteries. This is further compounded by the effect of gravity. To mitigate this problem veins, have valves at different intervals along the vein. Veins valves open and close spontaneously to assist the return of blood to the heart. This ideally occurs in a one-way direction towards the heart. Venous disease or venous insufficiency occurs when these valves become damaged. This leads to backward flow of blood in the veins, resulting in increased venous pressure in the downstream and leakage of fluid into the soft tissue causing swelling, heaviness, fatigue, restless legs and skin changes. Some of these veins buckle under this increased pressure to become varicose and spider veins that can be seen coursing along the skin. If left untreated this disruption in blood return can cause significant pain, leg swelling, leg ulcers and general discomfort.
What causes damage to the valves?
Damage vein valves or what is generally referred to as venous insufficiency can be precipitated by known causes like advancing age (greater than 50), multiple pregnancies, morbid obesity (significant weight gain), smoking, jobs requiring prolonged standing or sitting, blood clots (superficial or deep vein thrombosis) and genetic anomalies (tendency to be more prominent in some families).
What are the symptoms of venous disease?
Venous disease can present itself in many ways. Some patients have mostly varicose and spider veins and others present with leg swelling or a combination of both in varying degrees of severity. Typical symptoms include aching or heaviness in the legs, leg cramps, swelling in ankles, fatigue, burning, itching, throbbing, restless legs especially at night, skin discoloration which may be dark, bronze or red and venous ulcers. While venous disease can cause cellulitis quite often many patients with venous disease are misdiagnosed as cellulitis. While some patients may experience severe symptoms others may be asymptomatic.
How common is venous disease?
The Society of vascular surgery estimates that more than 25 million adults in the United States suffered from chronic venous insufficiency with more than 6 million suffering from advanced disease. The annual cost of care is estimated at more than $3 billion. Chronic venous insufficiency accounts for the loss of more than 2 million workdays each year and with 12% of the patients seeking early retirement. It can affect men and women of all ages and activity levels, and while it has a strong genetic component, venous disease can be aggravated by environmental risks, pregnancy, and other factors. Venous disease is common in people who have jobs that require long periods of standing, and the risk of venous disease increases with age.
Are my varicose veins dangerous?
Varicose veins and leg swelling are very often due to poor flow in your veins with damaged valves or proximal vein obstruction with inability to timely return blood to your heart. Previously they were mostly considered cosmetic but with recent advances in science we know that there are symptoms of progressive disease in veins. They are a significant source of discomfort if left untreated. Eventually, varicose veins and venous insufficiency can lead to phlebitis, cellulitis and leg ulcers. Varicose veins can also be a source of embarrassment and continue self-awareness. This can erode self-esteem leading to social isolation and significant effects on the quality of life.
Are there complications associated with venous disease?
Venous disease tends to progress over time if left untreated. Slow skin changes can result in significant thickening of the skin and soft tissue, what is commonly referred to as lipodermatosclerosis. There are increased chances of superficial thrombophlebitis (clotting in the superficial veins), which at times can extend into the deep veins (deep vein thrombosis) and frequently causes severe pain and incapacitation. Spontaneous bleeding can also occur on exposed or injured varicose veins sometimes when doing routine chores like bathing. Chronic venous hypertension can lead to recurrent ulceration with significant oozing of fluid from these leg ulcers that are very slow to heal. It makes it difficult for patients to wear clothes or shoes and can become a frequent source of embarrassment.
How are varicose veins and chronic venous insufficiency diagnosed?
Varicose veins and chronic venous insufficiency diagnosed by obtaining an adequate history from the patient and performing a rigorous physical exam. The findings are confirmed by venous duplex ultrasound to assess valve function, blood flow and proximal vein anatomy.
What is Deep Vein Thrombosis and how do I prevent it?
A clot that occurs in a deep vein is referred to as a deep vein thrombosis (DVT). This can be a serious, life-threatening condition that requires immediate medical care. If the clot breaks free it can travel in your body to your lungs where it is called a Pulmonary Embolism. Sitting in a confined space or traveling for long periods can increase the risk of DVT, but many other factors contribute to its risk, including inherited disorders, certain medications or vein injuries.
Steps you can take to prevent DVT include wearing compression stockings during long plane rides or periods of being stationary and moving regularly during long periods or sitting. Talk with your doctor or contact the Vein Healthcare Center for additional prevention techniques and lifestyle changes that will help reduce your risk of DVT.
If I have symptoms of venous disease, am I at risk for Deep Vein Thrombosis?
While symptoms of venous disease can increase the chances of experiencing superficial venous thrombophlebitis or clotting in the superficial veins, there is no indication that those who experience venous disease will have deep vein thrombosis, nor is DVT a symptom of the progression of venous disease. However, irritation of the vein wall, which occurs in superficial venous thrombophlebitis, can be a risk factor for DVT.
Is there a cure for venous disease?
Venous disease is generally a chronic progressive disease that is treatable but not completely curable. It seldom leads to limb loss but can be a persistent nuisance and a source of discomfort if not well-managed can contribute to overall poor health and wellbeing.
Are there steps I can take to alleviate my symptoms of venous disease?
Yes. Blood flow in veins is typically much more sluggish than in arteries. Anything that impedes blood flow such as weight gain particularly around the midsection, sedentary lifestyle, smoking, pregnancy, long car or plane rides can exacerbate venous disease. Measures such as exercise, leg elevation above the heart, loose fitting clothing, proper shoes (avoiding high heels), frequent breaks if sitting for prolonged periods of times, proper hydration and the use of graduated compression stockings can help support smooth return of blood to the heart and mitigate venous insufficiency.
What treatments options are available?
Treatment typically begins with making the proper diagnosis and attempts to identify some of the causes of the venous insufficiency. Regular exercise, weight loss, leg elevation and graduated compression stockings have been found to help with symptoms. Breakthroughs and minimally invasive often office-based procedures have resulted in many treatment options for patients. These procedures offer less treatment time, less pain, convenient scheduling and elimination of discomfort. For patients with severe chronic pain or recurrent ulcers and constant weeping, treatment can be life changing.
What are my options for treatment?
Endovenous laser ablation (EVLA) also known as endovenous laser therapy (EVLT) and radiofrequency ablation (RFA) has become the main minimally invasive office-based procedures used in the treatment of venous insufficiency and varicose veins causing leg pain and other symptoms described above. Both procedures apply direct heat to the inside of the vein which causes them to shrink, scar down and eventually disappear ( hence “vein closure procedure”). Following closure of incompetent veins blood flow is rechanneled into many other dormant veins with healthy valves. Other treatment options like ambulatory phlebectomy remove larger veins from the skin surface through small, tiny incisions. Sclerotherapy involves injecting medication into the vein which induces scaring, sealing the small veins and making them fade away.
Are these treatments covered by insurance?
Most insurance plans cover treatment for symptomatic varicose veins and leg swelling, especially if they cause pain or complications. Cosmetic-only procedures may not be covered. All patients with venous disease experiencing symptoms described above fit the criteria of medical necessity, which includes lifestyle disruption, pain, and complications if the disease is allowed to progress. Some insurance companies require prior authorization which can be obtained by your primary care physician or Fayetteville Vascular and Vein Center staff member on your behalf.
What are the success rates of venous treatment?
Current renovations in equipment and treatment modalities have resulted in excellent initial and long-term success rates when performed by well-trained vascular surgeons. Endovenous laser therapy and the radiofrequency ablation both have success rates between 94 to 98% at 5 years.
Can varicose veins come back after treatment?
Yes, especially if underlying risk factors persist. Follow-up care and lifestyle changes such as smoking cessation, exercise, maintaining healthy weight and the use of graduated compression stockings help reduce recurrence.
Are spider veins the same as varicose veins?
No. Spider veins are smaller, superficial veins that appear red, blue, or purple. They’re usually cosmetic and less symptomatic than varicose veins
Can men get varicose veins?
Yes. Though more common in women, about 45% of men will develop varicose veins during their lifetime.
Are there risks associated with treatment?
All medical procedures have some risk associated with them. Endovenous laser therapy or radiofrequency ablation are considered very safe procedures with extremely low risk. Typical complications related to the procedure include infection and deep vein thrombosis which occur in less than 1% of the patients. Follow up Duplex ultrasound studies are obtained within 1 week of the procedure to confirm closure of the veins and rule out clot extension into the deep veins. If such extension is found, which is very infrequent, the patient is immediately placed on new generation blood thinners with hardly any need for hospitalization. Another ultrasound is done after 2 weeks and if the clot is noted to have disappeared the patient is taken off the blood thinners.
Are there age restrictions for endovenous treatment?
Ambulatory patients ranging in age from the teens to the ninties can all benefit from vein treatment. These treatments are generally minimally invasive and rarely require a general anesthetic. A proper diagnosis quite often is all that is required.
Do vein procedures require a hospital stay?
At Fayetteville Vascular and Vein Center most treatment for venous insufficiency is performed on an outpatient basis with very minimal downtime and very few postoperative restrictions. 99% of our patients resume activity or return to work the following day. Since we used sedation for these procedures, we insist that the patient be driven to and from the procedure by friends, family members or arranged public transportation. Patients are also advised to avoid operating any heavy machinery till the following day.
Can I receive treatment if I take blood thinners or chronic pain Medications?
Yes, you can. We rarely need to stop your blood thinners for the procedures. Sometimes not stopping them might be advantageous to you since they decrease the very small but possible risk of deep vein thrombosis. Always inform your caregiver about all medications that you are taking.
How soon will my pain, discomfort and varicose veins go away after treatment?
Most patients generally report an immediate relief of their symptoms following the procedure. Many of the varicose veins disappear or shrink and symptoms such as heaviness, fatigue, aching, itching and restlessness improved significantly following treatment. It is important, however, to note that maximum benefit occurs over time and in some cases could take several months for the veins or leg discoloration to disappear. Some of the varicose and spider veins may require additional treatment like sclerotherapy to completely disappear.
How long is the recovery time after treatment?
For procedures performed in the morning we generally advise patients to walk for about 1 to 1-1/2 hours in the afternoon. We recommend taking the dressing off the following day. Patients can resume work the following day. For 4 to 5 days following treatment, it is recommended that you avoid strenuous exertion such at the gym, running, hot tubs and heavy lifting.
In addition to endovenous treatment, are there other treatment options?
While minimally invasive endovenous thermal ablation therapies have become quite available, noninvasive options such as compression stockings, exercise, lifestyle changes and prevention techniques are also available. At Fayetteville Vascular and Vein Center, we can customize a treatment plan that suits your lifestyle.
Questions About Your Visit to Fayetteville Vascular and Vein Center
Do I need a referral from my primary care physician?
Check with your insurance provider to confirm whether a not a referral from your primary care physician is required. You are also welcome to schedule an appointment without involving your primary physician.
What should I expect from my visit to Fayetteville Vascular and Vein Center?
Initial visits to Fayetteville Vascular and Vein Center usually take about 45 minutes to 1 hour. This includes filling intake forms and a consultation with Dr. Leke. This visit is intended to provide a comfortable environment where you have an opportunity to learn about your condition and ask some very important questions about your treatment options. Dr. Leke may request further studies such as a venous duplex ultrasound of your legs which are generally performed on a different date at the same facility. These studies allow Dr. Leke to gauge the severity of your venous insufficiency and tailor his treatment recommendations to your specific needs.
How do I prepare for my procedures( EVLA/Sclerotherapy/Ambulatory Phlebectomy)?
Dr. Leke will engage in a thorough discussion of the procedure with you. The patient information section at the clinic will provide you with written instructions to help you prepare for your return visit to Fayetteville Vascular and Vein Center and guidelines to observe following your treatment.
Where is the Fayetteville Vascular and Vein Center located?
The Fayetteville Vascular and Vein Center is located at 3410 Village Dr, Suite 200, Fayetteville, NC 28304. We covered the greater Fayetteville area and surrounding counties.
Some important facts about Venous Disease
Venous Disease & the Primary Care Practice
The United States has one of the highest incidences of venous disease. Most of this is attributed to the rising incidence of morbid obesity. This has become a significant public health issue with billions of dollars spent annually on management of venous disease.
Venous disorders encompass has a wide range of conditions ranging from superficial and deep venous insufficiency, varicose veins and superficial and deep venous thromboembolism. Symptoms may include leg pain, throbbing, heaviness, cramps, restlessness or discoloration. Some patients may experience nonhealing ulcers which may be recurrent, cellulitis or phlebitis. Still some patients may be asymptomatic or fail to tie their conditions to venous insufficiency
Significant advancement in technology has greatly improved outcomes which previously were quite discouraging and left many patients without good options. Several decades ago, vein striping was considered the gold standard for management of venous insufficiency. Today it is rarely performed, replaced by more successful minimally invasive techniques such as EVLT, RFA, sclerotherapy and stab phlebectomy. These very innovative treatment options, performed with local anesthesia, in an office setting, with long-term treatment success rates of more than 94%, have greatly revolutionized treatment and changed the way the medical community perceives venous disorders.
Facts About Venous Disease
- Venous disease affects your patients. It is estimated that more than 80 million Americans have some form of venous disease.
- Venous disease is one of the most common chronic conditions in North America and Western Europe. This appears to mirror the incidence of morbid obesity and an increasingly sedentary lifestyle.
- An estimated 25-40 million people suffer from their symptoms.
- U.S. estimate for venous disease: 55% in females and 40-45% in males.
- Visible varicose veins: 20 to 25% of women compared to 10 to 15% of men
- 70% of American women and 40% of men will experience varicose veins symptoms by the time they reach their sixties.
- Some people with venous disease present with no symptoms, only skin changes and/or bulging veins.
- Gender and age are two primary risk factors in the development of venous insufficiency.
- Individuals who have been pregnant more than once, have a family history of varicose veins, or spend a great deal of time standing significantly increase their risk of the disease.
- Venous disease can be a factor in chronic leg cramping or restless leg syndrome.
- Varicose veins hardly ever go away without treatment and usually progress over time. Symptoms and progression can be controlled with weight maintenance, exercise and graduated compression garments.
- Symptoms of venous disease result in millions of lost workdays per year.
- Venous diseases can occur at almost any age.
Venous Disease as a Component of Patient Care
Physicians and other caregivers who manage patients with or at risk of venous insufficiency at the forefront of reducing this affliction in a growing number of patients suffering from symptoms. This can be done by providing patients with the latest information on modern approaches to testing, diagnosis and treatment. By such endeavors the medical community can make an important contribution towards improving the well-being and quality of life of millions across the country.
A Population at Risk
Common venous disorders are still undiagnosed and undertreated. Many patients experience chronic symptoms such as leg pain, sleeplessness, discomfort and social isolation. Quite often most of these patients are not aware that venous disorders are progressive and as such their symptoms intensify, leading to very serious complications. Unsightly varicose veins and chronic leg ulcers decrease their engagement in social activities, erode self-confidence and ultimately result in poor health and general wellbeing.
It is all too common to see patients who consider varicose veins as mostly a cosmetic problem and do not seek treatment. It is also common to see patients with strenuous jobs requiring prolonged standing who think that fatigue and chronic leg pain is simply a part of life. Men suffer from more advanced venous disease because they are less likely to seek treatment for pain, fatigue, leg swelling or varicosities.
Options for Care
Many elderly patients still assume that invasive options remain the standard of care. As a result of that most of them have generally not pursued treatment because of such assumptions. Many do not realize that treating the source of venous insufficiency can prevent subsequent complications such as phlebitis, chronic pain, worsening appearance such as discoloration, edema and recurrent leg ulcers.
Vein Health as Part of Overall Care
The grim statistics of venous disease can only be improved by integrating venous health in the overall care of our patients. By integrating venous health into physical examinations or as part of general health concerns, and by making venous system health a priority in treating those at risk or with early stage symptoms, fewer patients will suffer from this disease.
The Primary Physician and caregiver’s Role in Advancing Vein Care
Primary physicians and caregivers who see patients as part of their practice play a central role in advancing the understanding of venous disease. When patients understand their disease and are informed about options for treatment, they are more likely to have a positive interaction with their provider, receive quality care, and improve their quality of life.
What You Can Do as a Primary Care Physician or caregiver
• Know the risk factors of venous disease.
• Know the population most at risk.
• Ask patients about their symptoms.
• Inform patients with symptoms of venous disease about treatment options
• Inform patients who may be at risk about their options for screenings, prevention, and treatment.
• Tell patients how to prevent or alleviate venous symptoms and how to decrease their risk of deep vein thrombosis.
• Inform patients who may have had previous treatment, or those who have been dissatisfied with traditional, more invasive approaches, about today's treatment options.
• Maintain a current Knowledge base venous risk venous risks, symptoms, and treatment as well as advances in venous care.
• Provide an information sheet to patients with risk factors or symptoms of venous disease.
• Refer patients to a certified vein specialist.
• Contact Fayetteville Vascular and Vein Center with any questions about vein health or to learn more about venous disease.
Importance of a Vein Specialist
Venous disorders are caused by structural and biochemical abnormalities of the vein wall that with progression, lead to varicose veins, pain and swelling, clots, vein bleeding and ulcers. Long-standing varicose veins can lead to vein failure in the "bridging" or perforator veins. As a result, those with varicose veins are more likely to develop advanced symptoms such as increased pain, skin changes, and ultimately, ulcers. Because of its progressive nature, treating venous disease is rarely simply cosmetic, and requires comprehensive care by a specialist.
Treating the Source
It is important that patients experiencing symptoms, requesting evaluation, or inquiring about cosmetic vein removal receive a referral to a vein specialist who can assess the source of the insufficiency and provide professional medical care. While the presence of a vein insufficiency can often be diagnosed in the superficial vein, only comprehensive examination by a vascular surgeon can identify the source of insufficiency. The use of venous ultrasound is critical for the detection of venous insufficiency at its source. Ultrasound mapping and interpretation by a highly skilled vascular sonographer is paramount to receiving an accurate diagnosis.
Referring Patients to Fayetteville Vascular and Vein Center
Dr. Michael Leke, MD I has been a practicing vascular surgeon in the Fayetteville area for the last 18 years, providing outstanding medical treatment in all aspects of vein health for patients in all stages of venous disease. Part of this mission is to provide good resource for physicians and medical professionals who are seeking information about the latest trends and research in venous care and treatment, those interested in opportunities for doctor-to-doctor consultation about areas of vein health, and those seeking a trusted referral source.
Our commitment at Fayetteville Vascular and Vein Center
Dr. Leke is committed to advancing the level of communication between specialist and primary physicians and contributing to a collaborative environment as it relates to patient care. This commitment extends to full doctor consultation and disclosure of patient treatment and health management. He extends every effort that makes a contribution to better, more complete patient care.
Easy Referral for All Patient Concerns
Dr. Leke welcomes the opportunity for referrals from all physicians and medical professionals in the Fayetteville greater community. Physicians who have patients that may be new to vein treatment, and those who have had previous experiences with vein specialists and have been dissatisfied with traditional, more invasive approaches to treatment are encouraged to contact Fayetteville Vascular and Vein Center
Patient Referrals
Thank you for referring your patients to Fayetteville Vascular and Vein Center. We are pleased to serve as a resource for all physicians wishing to provide their patients with outstanding care for their venous disorders.
If you are a healthcare provider interested in referring a patient to the Vein Healthcare Center, please download the referral form by clicking here.
If you have questions or need additional information, please call
Fayetteville Vascular and Vein Center at
910 401 0202.
Schedule a Consultation With Dr. Leke for Vein & Vascular Care in Fayetteville
If you’re experiencing varicose veins, leg swelling, or other vascular concerns, contact Dr. Michael Leke today for a professional evaluation. We’ll help you find the right treatment to restore your comfort and vascular health.
📞
Phone:
910-401-0202
